Instead of talking about single payer health care in the abstract (“wouldn’t it be nice if health care were free?”), let’s discuss a concrete case of a single payer health care system. Canada’s health care system is a pure government-funded system. Canadian residents pay money into the system via taxation. And when they get sick, they go into a government-run hospital and ask for government-run health care. The idea of single payer health care makes a lot of politicians feel good, and it draws applause when they talk about it in the abstract. But forget the abstract. How well does it work in reality?
Here’s an article from a Canadian health care policy expert, Sally C. Pipes.
She writes:
The Canadian single-payer regime subjects thousands of patients to life-threatening delays for treatment.
Our northern neighbors’ wait times grow longer with each passing year. According to the Fraser Institute, a Canadian think tank, the typical patient in need of specialist treatment last year waited 21.2 weeks after referral from a general practitioner — a record high. In 1993, the median wait time was less than half that figure — 9.3 weeks.
In British Columbia, the median wait is even longer — a grand total of 26.5 weeks from referral from a general practitioner to receipt of treatment from a specialist. That’s more than half a year.
Lengthy delays are a hallmark of single-payer. Demand for care is essentially limitless when someone else is paying the bill.
But the provincial and federal governments in Canada don’t have limitless resources. So they typically set a global budget for care. Doctors and hospitals can only provide so much care before their costs exceed their revenue from the government. And they can only afford to keep a limited amount of equipment operational, such as MRI machines or CT scanners.
Demand for care inevitably outstrips supply. So the government has to establish wait lists.
Long waits aren’t merely inconvenient; they’re dangerous. Consider the case of Walid Khalfallah, a British Columbian boy with severe scoliosis profiled by the Vancouver Sun in 2012. The Sun reported that he faced a three-year wait for spinal surgery, even though medical guidelines recommended a maximum wait of three months.
Delays can even prove fatal. Long waits have contributed to the deaths of more than 44,000 Canadian women in the past two decades, according to a Fraser Institute study.
Many patients would gladly pay extra to receive care more quickly. But British Columbian law makes it effectively impossible to do so.
The hardest thing to explain to Americans who are only familiar with private insurance is that if the government tells you no in a single-payer system, your only option is to take whatever money you have left (after being taxed for the single-payer system) and go outside the country. A lot of Canadian socialist politicians do exactly that, when they need reliable health care. Like Bernie Sanders, they say one thing to their naive followers, and do something else in their private lives.
So how good is American health care? Maybe Canadians are waiting in line because their health care is so much better than ours.
American health care
One of the best health care policy experts writing today is Avik Roy, who writes for Forbes magazine.
Here is a recent column, which I think is useful for helping us all get better at debating health care policy.
Excerpt:
It’s one of the most oft-repeated justifications for socialized medicine: Americans spend more money than other developed countries on health care, but don’t live as long. If we would just hop on the European health-care bandwagon, we’d live longer and healthier lives. The only problem is it’s not true.
[…]If you really want to measure health outcomes, the best way to do it is at the point of medical intervention. If you have a heart attack, how long do you live in the U.S. vs. another country? If you’re diagnosed with breast cancer? In 2008, a group of investigators conducted a worldwide study of cancer survival rates, called CONCORD. They looked at 5-year survival rates for breast cancer, colon and rectal cancer, and prostate cancer. I compiled their data for the U.S., Canada, Australia, Japan, and western Europe. Guess who came out number one?
Here is the raw data:
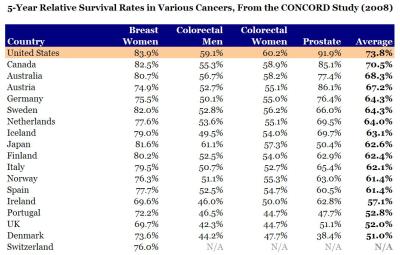
Click here to see the larger graph.
So, what explains this?
The article continues:
Another point worth making is that people die for other reasons than health. For example, people die because of car accidents and violent crime. A few years back, Robert Ohsfeldt of Texas A&M and John Schneider of the University of Iowa asked the obvious question: what happens if you remove deaths from fatal injuries from the life expectancy tables? Among the 29 members of the OECD, the U.S. vaults from 19th place to…you guessed it…first. Japan, on the same adjustment, drops from first to ninth.
It’s great that the Japanese eat more sushi than we do, and that they settle their arguments more peaceably. But these things don’t have anything to do with socialized medicine.
Finally, U.S. life-expectancy statistics are skewed by the fact that the U.S. doesn’t have one health-care system, but three: Medicaid, Medicare, and private insurance. (A fourth, the Obamacare exchanges, is supposed to go into effect in 2014.) As I have noted in the past, health outcomes for those on government-sponsored insurance are worse than for those on private insurance.
To my knowledge, no one has attempted to segregate U.S. life-expectancy figures by insurance status. But based on the data we have, it’s highly likely that those on private insurance have the best life expectancy, with Medicare patients in the middle, and the uninsured and Medicaid at the bottom.
Certainly, the life expectancy in our 100% government-run health care system, the Veteran’s Affairs health care system, is really, really low. They just kill the patients, give themselves bonuses, and then cover-up their failures when the investigators come.
I know that my readers who like to dig deep into economics and policy will love the links at the bottom of the article:
For further reading on the topic of life expectancy, here are some recommendations. Harvard economist Greg Mankiw discusses some of the confounding factors with life expectancy statistics, citing this NBER study by June and Dave O’Neill comparing the U.S. and Canada. (Mankiw calls the misuse of U.S. life expectancy stats “schlocky.”) Chicago economist Gary Becker makes note of the CONCORD study in this blog post. In 2009, Sam Preston and Jessica Ho of the University of Pennsylvania published a lengthy analysis of life expectancy statistics, concluding that “the low longevity ranking of the United States is not likely to be a result of a poorly functioning health care system.”
If we’re going to discuss health care, then let’s discuss facts. We shouldn’t be picking a health care system from the campaign speeches of politicians who tell us that we can keep our doctor, and keep our health plan, and our premiums will go down. We tried electing a charismatic deceiver in 2008, and it didn’t work out. We lost our doctors, lost our health plans, and our premiums went up enormously. We can do better than single-payer health care. We can do better than socialism.

When I was diagnosed with cancer last year I was so grateful to have rapid responses and treatment.
LikeLike
With single payer healthcare the government is highly incentivized to put people on waiting lists so they die before treatment.
LikeLiked by 1 person
That leaves them more money to buy votes with. They can spent the amount they save by killing the elderly on sex changes and abortions.
LikeLiked by 2 people
With more medical advances it has made it so once simplistic ideas of basic doctor visits to help people are replaced by expensive procedures that didn’t even exist years back.
I don’t see it as a failure to either Medicare or the US system that not all people can get help to one hundred percent.
The promise of science making it so we can all live really long was a lie and not financially feasible in the long run.
LikeLike